Epic AI Charting launches alongside new AI features
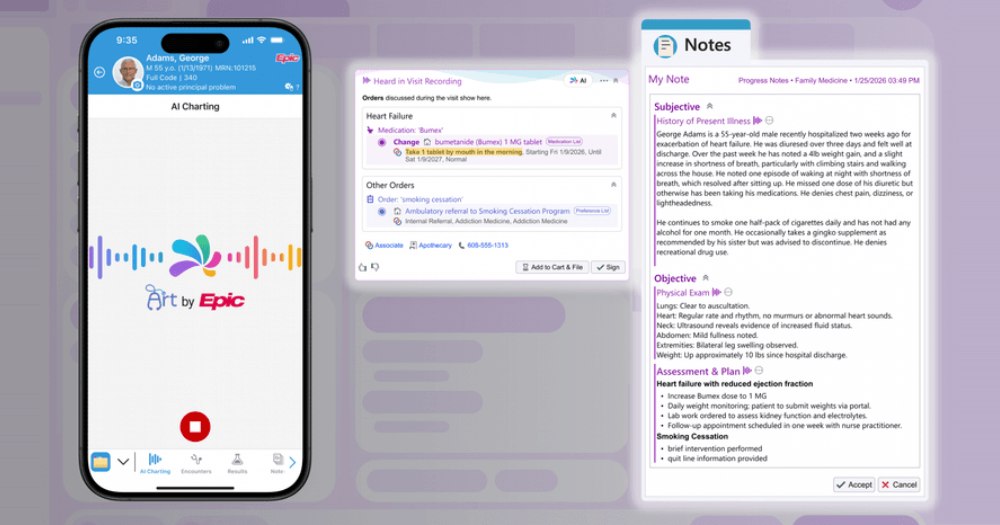
Epic Systems has launched a long-anticipated built-in AI feature called AI Charting that promises to upend how clinicians document care. The tool listens to conversations during patient visits, drafts clinical notes on the fly, and even queues suggested orders based on the discussion. The goal is blunt and straightforward. Free clinicians from paperwork so they can focus on patients.
Epic positions this as the next frontier in electronic health records, folding artificial intelligence directly into the core of its platform rather than bolting it on later.
How does it work?
AI Charting is part of Epic's broader AI suite, branded as Art for clinicians. It captures spoken conversations in real time, transcribes them, and turns them into structured clinical documentation. The magic isn't just transcription. It's integration. Because AI Charting lives inside Epic's software, it has immediate access to a patient's longitudinal record — medications, history, previous visits — and uses that context to draft notes that make clinical sense.
Here's what it does today:
- Real-time documentation while clinicians and patients talk
- Draft notes and orders based on that same conversation
- Voice commands let clinicians shape future notes — like "format the history as bullet points" — without lifting a finger from the exam room workflow
Epic's Corey Miller, vice president of research and development, captures the ethos: "Feedback has been very positive, and we're iterating quickly based on what clinicians tell us works best."
AI Charting doesn't stand alone. It sits beside Penny, an AI assistant for operational workflows like billing and denial appeals, and Emmie, a conversational AI for patients that lives in MyChart.
Why does it matter?
Healthcare has a paperwork problem. Clinicians can spend half their day typing notes and wrestling with electronic charts. Ambient AI promises to dramatically reduce that burden. By drafting notes during visits, AI Charting can save clinicians hours each week and shrink the infamous "pajama time" many endure after clinic hours.
This matters for clinicians and patients alike. When the clinician keeps their eyes on the person in front of them, the human connection deepens. Documentation doesn't become an afterthought. And hospitals and health systems see real gains too. Revenue cycle teams using Penny are reporting fewer coding denials and faster appeal letter creation.
There's a ripple effect, too. Third-party AI scribe vendors that sell standalone tools now have to compete with embedded functionality that taps deeply into Epic's data. Health systems are reevaluating expensive contracts with outside tools when Epic's native suite can do the heavy lifting in the record itself.
The context
Epic touches a huge portion of U.S. healthcare. Its electronic health record sits at the core of thousands of hospitals and clinics. The decision to build AI natively into that platform signals a broader shift in how healthcare IT is evolving. Instead of bolted-on features, intelligence lives where the data already lives.
This comes as ambient AI tools grow in popularity across the industry, with startups and legacy tech companies alike racing to offer scribes, assistants, and workflows that cut down documentation time. But Epic's advantage is its scale and integration. Its version of AI Charting isn't a separate overlay. It's woven into the daily tech clinicians already use.
For scribes and third-party developers, that's a game changer. Those who thrived by plugging into EHRs now face a platform where the vendor itself offers the same service. It raises the bar for what outside tools must offer — more specialization, deeper insight, or clear value that a native feature can't match.
💡Did you know?
You can take your DHArab experience to the next level with our Premium Membership.👉 Click here to learn more
🛠️Featured tool
 Easy-Peasy
Easy-Peasy
An all-in-one AI tool offering the ability to build no-code AI Bots, create articles & social media posts, convert text into natural speech in 40+ languages, create and edit images, generate videos, and more.
👉 Click here to learn more


